Why a generic insulin-resistance meal plan is not enough for PCOS
Most insulin-resistance meal plans circulating online were designed for prediabetes and type 2 diabetes. They focus on glucose load, fiber, and modest calorie reduction. They are not wrong, but they leave out three things that change everything in PCOS: the androgen-insulin feedback loop, the cortisol and HPA-axis interplay, and the inflammation gradient. A PCOS-aware insulin-resistance meal plan accounts for all three. It looks similar on the plate to a generic IR plan but it is calibrated differently — slightly higher protein, more attention to anti-inflammatory fats, more conservative fasting windows, and earlier carb timing in the day.
The androgen-insulin loop
Insulin and ovarian androgen production are tied. Hyperinsulinemia directly stimulates theca cells in the ovary to produce more testosterone. Insulin also suppresses sex hormone-binding globulin (SHBG), raising the proportion of free, biologically active testosterone. This is why insulin sensitization (through diet, exercise, or medication) reduces androgen excess in most PCOS women within 12 to 24 weeks. Cutting insulin spikes is the single highest-leverage dietary lever for PCOS, full stop.
Cortisol and HPA-axis interplay
Stress and disrupted sleep raise cortisol. Cortisol raises glucose, which raises insulin, which feeds back into the androgen loop. PCOS women, particularly lean PCOS and post-pill phenotypes, frequently have elevated baseline cortisol and exaggerated cortisol responses to stressors. This is why aggressive fasting (16+ hour windows), severe calorie restriction, and very low carbohydrate diets often backfire in PCOS even when they "work" for general insulin resistance: they raise cortisol, which raises insulin, which raises androgens.
Inflammation and the insulin signal
Low-grade chronic inflammation is present in most PCOS phenotypes (elevated CRP, IL-6, TNF-alpha). Inflammatory cytokines impair insulin signaling at the cellular level, which makes insulin resistance worse independent of carb intake. This is why anti-inflammatory dietary patterns (Mediterranean-style, with abundant omega-3s, polyphenols, and fiber) outperform pure carb restriction in head-to-head PCOS dietary trials.
The five rules of a PCOS-IR meal plan
1. Protein at every meal: 25-30 grams floor
Protein is the macronutrient most consistently associated with reduced insulin response, increased satiety, and improved body composition in PCOS. The 2023 International Evidence-based Guideline supports protein at 25 to 30 percent of energy intake, which translates to roughly 25 to 35 grams per meal across three meals plus a snack. For most women this is meaningfully more protein than they currently eat.
Practical: a "protein-anchored plate" approach. Build every meal around the protein first, then add vegetables, fat, and a measured starch. Examples: 4 oz salmon + sautéed greens + half cup quinoa + olive oil. Two eggs + half cup cottage cheese + berries + 2 tbsp walnuts. 5 oz chicken thigh + roasted vegetables + half a sweet potato + tahini sauce.
2. Carb timing: earlier in the day, paired
Insulin sensitivity is highest in the morning and declines through the day. Larger carb portions tolerated at breakfast and lunch are often less well tolerated at dinner. The 2013 Jakubowicz et al. trial in obese PCOS women (Tel Aviv University) showed that shifting calories toward breakfast (980 kcal breakfast, 640 lunch, 190 dinner) over 12 weeks reduced fasting insulin by 56 percent, reduced testosterone by 50 percent, and increased ovulation rate, compared to a calorie-matched control with calories shifted toward dinner. The control group saw essentially no improvement in any PCOS marker.
Practical: front-load the day. Bigger breakfast and lunch, smaller dinner. Pair every carb with protein and fat to blunt the glucose response. Skip naked carbs (a piece of toast alone, a bowl of pasta alone, a glass of fruit juice with anything).
3. Fiber: 25-35 grams per day
Fiber slows gastric emptying, blunts post-meal glucose, feeds the gut microbiome, and supports estrogen elimination. Most American women average 12 to 16 grams of fiber per day, well below the PCOS-supportive target. Quick fiber targets: 1 cup berries (8g), 1 medium avocado (10g), half cup lentils (8g), 1 cup broccoli (5g), 2 tbsp chia seeds (10g).
4. Anti-inflammatory fats: daily omega-3
EPA and DHA omega-3 fatty acids reduce inflammatory cytokines and improve insulin signaling at the cellular level. The 2023 Guideline supports either fatty fish 2-3 times per week (salmon, sardines, mackerel) or a fish-oil supplement providing approximately 1,500 to 2,000 mg combined EPA + DHA daily. Plant ALA omega-3s (flax, chia, walnuts) are useful but the conversion to EPA/DHA is poor (under 5 percent), so they do not fully substitute.
5. Avoid HPA stressors: large fasting windows, low-fat diets, excess caffeine
Three patterns reliably backfire in PCOS even though they help generic insulin resistance: aggressive fasting (16+ hours), low-fat dieting, and high caffeine on an empty stomach. Each raises cortisol, which raises insulin, which sustains the androgen loop. Conservative starting point: a 12-hour overnight fast (e.g., dinner finished by 8 pm, breakfast by 8 am), no calorie restriction below 1,400 to 1,600 kcal/day in most cases, fat at 30 to 40 percent of energy, and caffeine consumed with food rather than on an empty stomach.
A 5-day insulin-resistance-focused PCOS meal plan
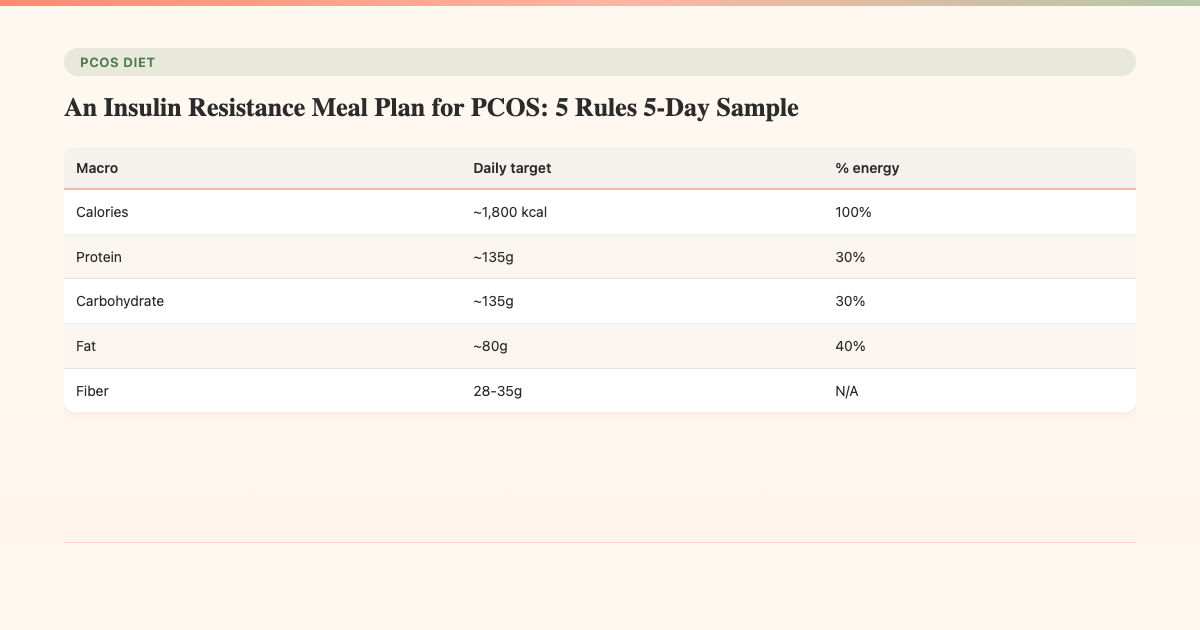
This sample plan targets approximately 1,800 kcal/day, with 30 percent carbs (~135g), 30 percent protein (~135g), and 40 percent fat (~80g). Adjust portions for your activity level and goals under your clinician's guidance.
Day 1 (Monday)
- Breakfast: 3-egg vegetable scramble with spinach, mushrooms, and feta + half avocado + 1 slice sourdough toast. (~30g protein, 25g carbs, 28g fat)
- Lunch: 5 oz grilled salmon over arugula and roasted vegetables + half cup quinoa + olive oil and lemon. (~38g protein, 35g carbs, 22g fat)
- Snack: Plain Greek yogurt (1 cup) + 12 almonds + 1/2 cup berries.
- Dinner: 5 oz baked chicken thigh + sautéed broccoli with garlic + half a roasted sweet potato + tahini drizzle. (~35g protein, 30g carbs, 18g fat)
Day 2 (Tuesday)
- Breakfast: Overnight oats: half cup rolled oats + 1 scoop whey or pea protein + 1 tbsp chia + half cup berries + 2 tbsp almond butter. (~32g protein, 38g carbs, 22g fat)
- Lunch: Mediterranean bowl: 5 oz grilled chicken + half cup chickpeas + cucumber, tomato, kalamata olives, feta + half cup quinoa + olive oil. (~40g protein, 38g carbs, 24g fat)
- Snack: 1 small apple + 2 tbsp natural peanut butter.
- Dinner: Sheet-pan dinner: 5 oz sirloin + roasted Brussels sprouts and red onion + half cup wild rice + chimichurri. (~38g protein, 30g carbs, 18g fat)
Day 3 (Wednesday)
- Breakfast: Smoked salmon plate: 3 oz smoked salmon + 2 hard-boiled eggs + cherry tomatoes + half avocado + 1 slice sprouted-grain toast. (~38g protein, 22g carbs, 26g fat)
- Lunch: Lentil soup (1.5 cups) + side green salad with olive oil and apple cider vinegar + 1 oz pumpkin seeds. (~28g protein, 40g carbs, 22g fat)
- Snack: 1 cup cottage cheese + 1/2 cup pineapple chunks.
- Dinner: Stir-fry: 5 oz tofu or chicken + mixed vegetables + half cup brown rice + sesame oil and tamari. (~32g protein, 35g carbs, 18g fat)
Day 4 (Thursday)
- Breakfast: Greek yogurt power bowl: 1.5 cups plain Greek yogurt + 1/2 cup granola + 1/2 cup berries + 2 tbsp ground flax + drizzle of honey (optional, 1 tsp). (~35g protein, 38g carbs, 18g fat)
- Lunch: Tuna salad (5 oz canned wild tuna in olive oil) over mixed greens + 1 boiled egg + half cup chickpeas + olive oil and lemon. (~40g protein, 22g carbs, 22g fat)
- Snack: Apple slices + 1 oz cheddar cheese + 12 almonds.
- Dinner: Salmon with roasted vegetables: 5 oz salmon + roasted asparagus and bell peppers + half cup farro + olive oil. (~38g protein, 32g carbs, 22g fat)
Day 5 (Friday)
- Breakfast: Veggie egg muffins (3) + 1/2 cup cottage cheese + 1/2 cup berries + 12 walnuts. (~32g protein, 18g carbs, 22g fat)
- Lunch: Bowl: 5 oz shredded chicken + cauliflower rice + black beans + salsa + avocado + lime + cilantro. (~40g protein, 30g carbs, 22g fat)
- Snack: Edamame (1 cup, in pods) + small handful pistachios.
- Dinner: Out-friendly: any grilled protein + double vegetables + skip the bread basket. If at home: shrimp scampi over zucchini noodles with olive oil and garlic.
Sample macros across the 5 days
| Macro | Daily target | % energy |
|---|---|---|
| Calories | ~1,800 kcal | 100% |
| Protein | ~135g | 30% |
| Carbohydrate | ~135g | 30% |
| Fat | ~80g | 40% |
| Fiber | 28-35g | N/A |
How to know if it is working: what to track over 8 weeks
- Energy and satiety. Within 1-2 weeks most women on this pattern report fewer mid-afternoon crashes and reduced sweet cravings. This is the earliest signal.
- Cycle response. If you have irregular cycles, look for increased frequency or shortened intervals over 2-3 cycles. Not everyone ovulates within 8 weeks; some take 12-16 weeks.
- Skin and mood. Acne and mood typically improve over 4-8 weeks if the underlying driver was insulin-androgen.
- Lab markers (re-test at 12 weeks). Fasting glucose, fasting insulin (calculate HOMA-IR), HbA1c, total testosterone, free androgen index, SHBG, hs-CRP, and a lipid panel. Compare to your baseline.
- Body composition (not weight alone). Waist-to-hip ratio is more useful than scale weight in PCOS. Loss of visceral fat improves insulin signaling even at stable scale weight.
When to ask your doctor about metformin or inositol
If 12 weeks of consistent dietary change has not produced measurable improvement in HOMA-IR, fasting insulin, cycle regularity, or symptoms, the next step is a medication or supplement conversation. Both metformin (1,500-2,000 mg/day) and myo-inositol (4,000 mg/day, often paired with 100 mg D-chiro-inositol) have substantial evidence for insulin sensitization in PCOS. Each has trade-offs: metformin is more potent for severe insulin resistance and prediabetes but produces GI side effects in 20-30 percent of users; inositol is much better tolerated but slightly less potent for severe IR. Read our full evidence comparison and bring it to your endocrinologist or OB-GYN appointment.
How PCOS Meal Planner personalizes the plan
The 5-day plan above is a template. PCOS Meal Planner builds a personalized version of this every week based on your phenotype, current weight, activity, cycle phase, food preferences, allergies, and household size. Recipes auto-swap if you say you don't eat fish; macros auto-adjust if you log a higher activity day; the grocery list builds itself. Start a free 7-day trial.
Frequently Asked Questions
How long does it take to reverse insulin resistance with PCOS?
Most women see measurable improvements in HOMA-IR and fasting insulin within 8 to 12 weeks of consistent dietary change. Full reversal — when achievable — typically takes 6 to 12 months. Insulin resistance often improves before noticeable weight loss, which is why labs are a more reliable marker than the scale.
Can I eat fruit if I have insulin resistance with PCOS?
Yes. Whole fruit, especially berries, kiwi, citrus, and apples, is fine and even beneficial for most insulin-resistant PCOS women. Pair with protein or fat (berries with Greek yogurt, apple with peanut butter) to blunt the glucose response. Avoid fruit juices, dried fruits in large portions, and fruit-only smoothies.
Should I do keto for insulin-resistant PCOS?
Mixed evidence. Short-term ketogenic diets (8-12 weeks) show good metabolic improvements in PCOS — reductions in fasting insulin, HOMA-IR, and androgen levels. Long-term, very-low-carb diets can disrupt thyroid function, cortisol regulation, and cycle in some women. A moderate-carb (30-40 percent), Mediterranean-style approach is more sustainable for most PCOS women and produces comparable insulin-sensitivity benefits over 12 months.
What lab tests should I get to track PCOS insulin resistance?
Fasting glucose, fasting insulin (calculate HOMA-IR = glucose mg/dL × insulin mIU/L / 405), HbA1c, oral glucose tolerance test if your doctor recommends it, lipid panel, and inflammatory markers (hs-CRP). Repeat every 6 months while making changes. Add total testosterone, free androgen index, and SHBG if you're tracking the androgen-insulin loop.
Is intermittent fasting safe for insulin-resistant PCOS?
12 to 13 hour overnight fasts are generally safe for most PCOS women and may be modestly beneficial. Longer fasts (16+ hours) are mixed: they can improve insulin sensitivity in some women but worsen HPA-axis stress in others, particularly lean PCOS, post-pill PCOS, and women with disordered eating history. Try a 12-hour fast first and monitor sleep, mood, and cycle response over 8 weeks before extending.
Why did calorie cutting fail to help my PCOS weight?
Several reasons. Aggressive calorie restriction (under 1,200-1,400 kcal/day for most women) raises cortisol and worsens HPA-axis dysfunction, which feeds the insulin-androgen loop. Cutting fat in particular often raises insulin response by removing the macronutrient that blunts post-meal glucose. Cutting protein impairs muscle preservation and lowers metabolic rate. Protein-forward, moderate-carb, anti-inflammatory eating typically produces better results than low-calorie dieting in PCOS, often at higher daily intake.
Sources
- Teede HJ, Tay CT, Laven JJE, et al. Recommendations from the 2023 International Evidence-based Guideline for the Assessment and Management of Polycystic Ovary Syndrome. Fertility and Sterility. 2023;120(4):767-793. PubMed: 37580056
- Jakubowicz D, Barnea M, Wainstein J, Froy O. Effects of caloric intake timing on insulin resistance and hyperandrogenism in lean women with polycystic ovary syndrome. Clinical Science. 2013;125(9):423-432. PubMed: 23688334
- Diamanti-Kandarakis E, Dunaif A. Insulin resistance and the polycystic ovary syndrome revisited: an update on mechanisms and implications. Endocrine Reviews. 2012;33(6):981-1030. PubMed: 23065822
- Lim SS, Hutchison SK, Van Ryswyk E, Norman RJ, Teede HJ, Moran LJ. Lifestyle changes in women with polycystic ovary syndrome. Cochrane Database of Systematic Reviews. 2019;3(3):CD007506. PubMed: 30921478
- Moran LJ, Ko H, Misso M, et al. Dietary composition in the treatment of polycystic ovary syndrome. Journal of the Academy of Nutrition and Dietetics. 2013;113(4):520-545. PubMed: 23420000
- Barrea L, Arnone A, Annunziata G, et al. Adherence to the Mediterranean diet, dietary patterns and body composition in women with polycystic ovary syndrome (PCOS). Nutrients. 2019;11(10):2278. PubMed: 31547562
- American College of Obstetricians and Gynecologists. ACOG Practice Bulletin No. 194: Polycystic Ovary Syndrome. Obstetrics & Gynecology. 2018;131(6):e157-e171. PubMed: 29794677
- American Diabetes Association. Standards of Care in Diabetes. Diabetes Care. 2024;47(Suppl 1). Diabetes Care
- National Institutes of Health, Office of Dietary Supplements. Magnesium, Chromium, Vitamin D fact sheets. NIH ODS
Related reading on PCOS Meal Planner
- PCOS 101: Complete Dietitian-Reviewed Guide
- Inositol vs Metformin for PCOS
- The PCOS Grocery List
- Why Calorie Restriction Backfires in PCOS
- PCOS Breakfast Ideas
How this article was researched
This meal plan was built from the 2023 International Evidence-based Guideline for the Assessment and Management of PCOS, the 2019 Cochrane systematic review on lifestyle changes for PCOS, the Jakubowicz et al. (2013) breakfast-timing trial, and primary nutrition and endocrinology research in PubMed-indexed journals. This article is being prioritized for medical review by our contracted Registered Dietitian Nutritionist as part of our retroactive review program. See our editorial standards.
Community Comments
Add a comment